
BUNION:
Bunions are a common problem among women, and they can be painful part of everyday life. A bunion is a growth on the big toe near the base where it connects with the foot. The growth is due to soft tissue enlargement under the skin. Women frequently develop bunions either from wearing shoes that do not fit properly, or from high heels that actually do fit well. There are other causes of bunions, such as heredity and poor foot structure.
Even though bunions are a common foot deformity,
there are misconceptions about them. Many people
may unnecessarily suffer the pain of bunions for
years before seeking treatment.
What is a Bunion?
A bunion (also referred to as hallux valgus or hallux
abducto valgus) is often described as a bump on the
side of the big toe. But a bunion is more than that.
The visible bump actually reflects changes in the bony
framework of the front part of the foot. The big toe
leans toward the second toe, rather than pointing
straight ahead. This throws the bones out of alignment
– producing the bunion’s “bump.”
Bunions are a progressive disorder. They begin with a leaning of the big toe, gradually changing the angle of the bones over the years and slowly producing the characteristic bump, which becomes increasingly prominent. Symptoms usually appear at later stages, although some people never have symptoms.
Causes
Bunions are most often caused by an inherited faulty mechanical structure of the foot. It is not the bunion itself that is inherited, but certain foot types that make a person prone to developing a bunion.
Although wearing shoes that crowd the toes won’t actually cause bunions, it sometimes makes the deformity get progressively worse. Symptoms occur most often when wearing shoes that crowd the toes, such as shoes with a tight toe box or high heels. This may explain why women are more likely to have symptoms than men. In addition, spending long periods of time on your feet can aggravate the symptoms of bunions. Symptoms may therefore appear sooner.
Symptoms
Symptoms, which occur at the site of the bunion, may include:
-
Pain or soreness
-
Inflammation and redness
-
A burning sensation
-
Possible numbness
Some of the common ways bunions can be treated are:
-
Bunion pads – Bunion pads can help relieve pressure on the sensitive area. Your Santa Fe podiatrist will be able to recommend the correct pad for your bunion.
-
Moleskin – A moleskin patch covers the bunion and pressure areas. This protects the bunion from being rubbed by shoes, which can result in blisters and other complications.
-
Wide shoes – Wearing shoes that have a wide toe box will provide room for the area around the toes. Tight, narrow, or high-heeled shoes put pressure on the bunion, which causes pain.
-
Medications – Medication can be used to alleviate some of the pain and swelling that is associated with bunions.
-
Ice – As with other injuries, icing the area can relieve pain and reduce the swelling. Ice can be applied to the joint for 10-20 minutes at a time. The foot should be elevated higher than the heart while icing.
-
Surgery - May be necessary when bunion pain is intolerable, or affects your ability to wear shoes.
If you are experiencing bunions or other foot conditions, you need to seek the help of a knowledgeable foot and ankle specialist.
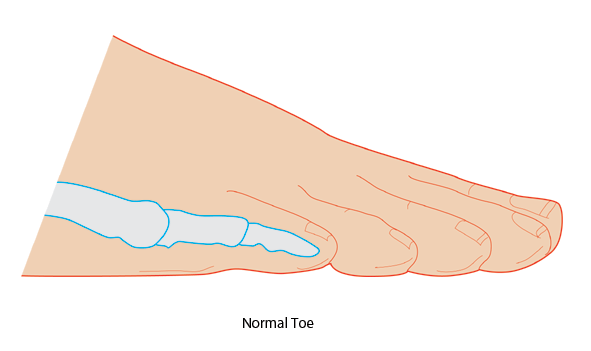


Hammertoes:
Usually stemming from muscle imbalance, this condition
occurs when the toe is bent into a claw-like position,
affecting most frequently the second toe, often
accompanying a bunion which slants the big toe toward
and under it. Painful corns or calluses candevelopeon the
top or bottom of the toe from the abnormal friction from
a shoe or sock.
What Is Hammertoe?
Hammertoe is a contracture (bending) of one or both
joints of the second, third, fourth, or fifth (little) toes.
This abnormal bending can put pressure on the toe
when wearing shoes, causing problems to develop.
Hammertoes usually start out as mild deformities and get progressively worse over time. In the earlier stages, hammertoes are flexible and the symptoms can often be managed with noninvasive measures. But if left untreated, hammertoes can become more rigid and will not respond to non-surgical treatment.
Because of the progressive nature of hammertoes, they
should receive early attention. Hammertoes never get
better without some kind of intervention.
Causes
The most common cause of hammertoe is a muscle/
tendon imbalance. This imbalance, which leads to a
bending of the toe, results from mechanical (structural)
changes in the foot that occur over time in some people.
Hammertoes may be aggravated by shoes that don’t fit
properly. A hammertoe may result if a toe is too long
and is forced into a cramped position when a tight shoe
is worn.
Occasionally, hammertoe is the result of an earlier
trauma to the toe. In some people, hammertoes are inherited.
Symptoms
Common symptoms of hammertoes include:
-
Pain or irritation of the affected toe when wearing shoes.
-
Corns and calluses (a buildup of skin) on the toe, between two toes, or on the ball of the foot. Corns are caused by constant friction against the shoe. They may be soft or hard, depending upon their location.
-
Inflammation, redness, or a burning sensation
-
Contracture of the toe
-
In more severe cases of hammertoe, open sores may form.
Diagnosis
Although hammertoes are readily apparent, to arrive at a diagnosis the foot and ankle surgeon will obtain a thorough history of your symptoms and examine your foot. During the physical examination, the doctor may attempt to reproduce your symptoms by manipulating your foot and will study the contractures of the toes. In addition, the foot and ankle surgeon may take x-rays to determine the degree of the deformities and assess any changes that may have occurred.
Hammertoes are progressive – they don’t go away by themselves and usually they will get worse over time. However, not all cases are alike – some hammertoes progress more rapidly than others. Once your foot and ankle surgeon has evaluated your hammertoes, a treatment plan can be developed that is suited to your needs.
Non-surgical Treatment
There is a variety of treatment options for hammertoe. The treatment your foot and ankle surgeon selects will depend upon the severity of your hammertoe and other factors.
A number of non-surgical measures can be undertaken:
-
Padding corns and calluses. Your foot and ankle surgeon can provide or prescribe pads designed to shield corns from irritation. If you want to try over-the-counter pads, avoid the medicated types. Medicated pads are generally not recommended because they may contain a small amount of acid that can be harmful. Consult your surgeon about this option.
-
Changes inshoewear. Avoid shoes with pointed toes, shoes that are too short, or shoes with high heels – conditions that can force your toe against the front of the shoe. Instead, choose comfortable shoes with a deep, roomy toe box and heels no higher than two inches.
-
Orthotic devices. A custom orthotic device placed in your shoe may help control the muscle/tendon imbalance.
-
Injection therapy. Corticosteroid injections are sometimes used to ease pain and inflammation caused by hammertoe.
-
Medications. Oral nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be recommended to reduce pain and inflammation.
-
Splinting/strapping. Splints or small straps may be applied by the surgeon to realign the bent toe.
When Is Surgery Needed?
In some cases, usually when the hammertoe has become more rigid and painful, or when an open sore has developed, surgery is needed.
Often patients with hammertoe have bunions or other foot deformities corrected at the same time. In selecting the procedure or combination of procedures for your particular case, the foot and ankle surgeon will take into consideration the extent of your deformity, the number of toes involved, your age, your activity level, and other factors. The length of the recovery period will vary, depending on the procedure or procedures performed.
Arch pain/ Heel Pain:
Heel pain is most often caused by plantar fasciitis, a condition that is sometimes also
called heel spur syndrome when a spur is present. Heel pain may also be due to other
causes, such as a stress fracture, tendonitis, arthritis, nerve irritation, or, rarely, a cyst.
Because there are several potential causes, it is important to have heel pain properly diagnosed.
A foot and ankle surgeon is able to distinguish between all the possibilities and determine the
underlying source of your heel pain.
Plantar Fasciitis
What Is Plantar Fasciitis?
Plantar fasciitis is an inflammation of the band of tissue (the plantar fascia) that extends from the heel to the toes. In this condition, the fascia first becomes irritated and then inflamed, resulting in heel pain.
Causes
The most common cause of plantar fasciitis relates to faulty structure of the foot. For example, people who have problems with their arches, either overly flat feet or high-arched feet, are more prone to developing plantar fasciitis.
Wearing non-supportive footwear on hard, flat surfaces puts abnormal strain on the plantar fascia and can also lead to plantar fasciitis. This is particularly evident when one’s job requires long hours on the feet. Obesity may also contribute to plantar fasciitis.
Symptoms
The symptoms of plantar fasciitis are:
-
Pain on the bottom of the heel
-
Pain in the arch of the foot
-
Pain that is usually worse upon arising
-
Pain that increases over a period of months
People with plantar fasciitis often describe the pain as worse when they get up in the morning or after they’ve been sitting for long periods of time. After a few minutes of walking the pain decreases, because walking stretches the fascia. For some people the pain subsides but returns after spending long periods of time on their feet.
Plantar Fibroma
What is the Plantar Fibroma?
A plantar fibroma is a fibrous knot (nodule) in the arch of the foot. It is embedded within the plantar fascia, a band of tissue that extends from the heel to the toes on the bottom of the foot. A plantar fibroma can develop in one or both feet, is benign (non-malignant), and usually will not go away or get smaller without treatment. Definitive causes for this condition have not been clearly identified.
Signs and Symptoms
The characteristic sign of a plantar fibroma is a noticeable lump in the arch that feels firm to the touch. This mass can remain the same size or get larger over time, or additional fibromas may develop.
People who have a plantar fibroma may or may not have pain. When pain does occur, it is often caused by shoes pushing against the lump in the arch, although it can also arise when walking or standing barefoot.
Diagnosis
To diagnose a plantar fibroma, the foot and ankle surgeon will examine the foot and press on the affected area. Sometimes this can produce pain that extends down to the toes. An MRI or biopsy may be performed to further evaluate the lump and aid in diagnosis.
Treatment Options
Non-surgical treatment may help relieve the pain of a plantar fibroma, although it will not make the mass disappear. The foot and ankle surgeon may select one or more of the following non-surgical options:
-
Steroid injections. Injecting corticosteroid medication into the mass may help shrink it and thereby relieve the pain that occurs when walking. This reduction may be only temporary and the fibroma could slowly return to its original size.
-
Orthotic devices. If the fibroma is stable, meaning it is not changing in size, custom orthotic devices (shoe inserts) may relieve the pain by distributing the patient’s weight away from the fibroma.
-
Physical therapy. The pain is sometimes treated through physical therapy methods that deliver anti-inflammatory medication into the fibroma without the need for injection.
If the mass increases in size or pain, the patient should be further evaluated. Surgical treatment to remove the fibroma is considered if the patient continues to experience pain following non-surgical approaches.
Surgical removal of a plantar fibroma may result in a flattening of the arch or development of hammertoes. Orthotic devices may be prescribed to provide support to the foot. Due to the high incidence of recurrence with this condition, continued follow-up with the foot and ankle surgeon is recommended.
Haglund’s Deformity
What is Haglund’s Deformity?
Haglund’sdeformity is a bony enlargement on the back of the heel. The soft tissue near the Achilles tendon becomes irritated when the bony enlargement rubs against shoes. This often leads to painful bursitis, which is an inflammation of the bursa (a fluid-filled sac between the tendon and bone).
Causes
Haglund’sdeformity is often called “pump bump” because the rigid backs of pump-style shoes can create pressure that aggravates the enlargement when walking. In fact, any shoes with a rigid back, such as ice skates, men’s dress shoes, or women’s pumps, can cause this irritation.
To some extent, heredity plays a role inHaglund’sdeformity. Inherited foot structures that can make one prone to developing this condition include:
-
A high-arched foot
-
A tight Achilles tendon
-
A tendency to walk on the outside of the heel.
Symptoms
Haglund’sdeformity can occur in one or both feet. The symptoms include:
-
A noticeable bump on the back of the heel
-
Pain in the area where the Achilles tendon attaches to the heel
-
Swelling in the back of the heel
-
Redness near the inflamed tissue
Diagnosis
After evaluating the patient’s symptoms, the foot and ankle surgeon will examine the foot. In addition, x-rays will be ordered to help the surgeon evaluate the structure of the heel bone.
Non-Surgical Treatment
Non-surgical treatment ofHaglund’sdeformity is aimed at reducing the inflammation of the bursa. While these approaches can resolve the pain and inflammation, they will not shrink the bony protrusion. Non-surgical treatment can include one or more of the following:
-
Medication. Oral nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be recommended to reduce the pain and inflammation.
-
Ice. To reduce swelling, apply an ice pack to the inflamed area, placing a thin towel between the ice and the skin. Use ice for 20 minutes and then wait at least 40 minutes before icing again.
-
Exercises. Stretching exercises help relieve tension from the Achilles tendon. These exercises are especially important for the patient who has a tight heel cord.
-
Heel lifts. Patients with high arches may find that heel lifts placed inside the shoe decrease the pressure on the heel.
-
Heel pads. Pads placed inside the shoe cushion the heel and may help reduce irritation when walking.
-
Shoe modification. Backless or soft backed shoes help avoid or minimize irritation.
-
Physical therapy. Physical therapy modalities, such as ultrasound, can help to reduce inflammation.
-
Orthotic devices. Custom arch supports control the motion in the foot.
-
Immobilization. In some cases, casting may be necessary.
When Is Surgery Needed?
If non-surgical treatment fails to provide adequate pain relief, surgery may be needed. The foot and ankle surgeon will determine the procedure that is best suited to your case. It is important to follow the surgeon’s instructions for post-surgical care.
Prevention
A recurrence ofHaglund’sdeformity may be prevented by:
-
Wearing appropriate shoes; avoid shoes with a rigid heel back
-
Using arch supports or orthotic devices
-
Performing stretching exercises to prevent the Achilles tendon from tightening
Ankle Sprain
What Is an Ankle Sprain?
An ankle sprain is an injury to one or more ligaments in the ankle, usually on the outside
of the ankle. Ligaments are bands of tissue – like rubber bands – that connect one bone
to another and bind the joints together. In the ankle joint, ligaments provide stability by
limiting side-to-side movement.
Some ankle sprains are much worse than others. The severity of an ankle sprain depends
on whether the ligament is stretched, partially torn, or completely torn, as well as on the
number of ligaments involved. Ankle sprains are not the same as strains, which affect
muscles rather than ligaments.
Causes
Sprained ankles often result from a fall, a sudden twist, or a blow that forces the ankle joint
out of its normal position. Ankle sprains commonly occur while participating in sports,
wearing inappropriate shoes, or walking or running on an uneven surface.
Sometimes ankle sprains occur because of a person is born with weak ankles. Previous
ankle or foot injuries can also weaken the ankle and lead to sprains.
Symptoms
The symptoms of ankle sprains may include:
-
Pain or soreness
-
Swelling
-
Bruising
-
Difficulty walking
-
Stiffness in the joint
These symptoms may vary in intensity, depending on the severity of the sprain. Sometimes pain and swelling are absent in people with previous ankle sprains. Instead, they may simply feel the ankle is wobbly and unsteady when they walk. Even if there is no pain or swelling with a sprained ankle, treatment is crucial. Any ankle sprain – whether it’s your first or your fifth – requires prompt medical attention.
Why Prompt Medical Attention Is Needed
There are four key reasons why an ankle sprain should be promptly evaluated and treated by a foot and ankle surgeon:
-
An untreated ankle sprain may lead to chronic ankle instability, a condition marked by persistent discomfort and a “giving way” of the ankle. Weakness in the leg may also develop.
-
A more severe ankle injury may have occurred along with the sprain. This might include a serious bone fracture that, if left untreated, could lead to troubling complications.
-
An ankle sprain may be accompanied by a foot injury that causes discomfort but has gone unnoticed thus far.
-
Rehabilitation of a sprained ankle needs to begin right away. If rehabilitation is delayed, the injury may be less likely to heal properly.
Ankle Sprain: Ankle sprains are caused by an unnatural twisting or force on the foot, which may stretch or tear of one or more ligaments on the of the ankle. If not properly treated, ankle sprains may develop into long-term problems. Symptoms of ankle sprains are pain, swelling, and bruising.
Treatment includes rest and elevate the ankle and apply ice to reduce swelling. A compressive ace-wrap may help to immobilize and support the injury during healing. Serious ankle sprains, particularly among competitive athletes, may require surgery to repair and tighten the damaged ligaments.
To prevent ankle sprains, try to maintain strength, balance, and flexibility in the foot and ankle through exercise and stretching, and wearing well-fitted shoes. Physical therapy may be helpful after an injury has healed to strengthen the weak ankle and prevent from reoccurring.
Plantar Fasciitus




Ankle Fracture:
. A broken ankle can involve one or more of the bones, as well as injury to the surrounding connecting tissues or ligaments. There are a wide variety of causes for broken ankles, most commonly a fall, an automobile accident, or sports-related trauma. Because a severe sprain can often mask the symptoms of a broken ankle, every ankle injury should be examined by a physician.
What Is an Ankle Fracture?
According to the American Academy ofOrthopaedicSurgeons, doctors have noticed an
increase in the number and severity of broken ankles since the 1970s, due, in part, to the
Baby Boomer generation being active throughout every stage of their lives.
A fracture is a partial or complete break in a bone. Fractures in the ankle can range from
the less serious avulsion injuries (small pieces of bone that have been pulled off) to
severe shattering-type breaks of the tibia, fibula, or both.
Ankle fractures are common injuries that are most often caused by the ankle rolling
inward or outward. Many people mistake an ankle fracture for an ankle sprain, but they
are quite different and therefore require an accurate and early diagnosis. They
sometimes occur simultaneously. A person may still be able to walk or put weight on
their foot. If you put weight or walk on a fractured or broken ankle, it is possible to
cause more damage or fracture the bone(s) further.
Symptoms
An ankle fracture is accompanied by one or all of these symptoms:
-
Pain at the site of the fracture, which in some cases can extend from the foot to the knee. No pain does not mean it isn’t a fracture.
-
Significant swelling, which may occur along the length of the leg or may be more localized.
-
Blisters may occur over the fracture site. These should be promptly treated by a foot and ankle surgeon.
-
Bruising that develops soon after the injury
-
Inability to walk—however, it is possible to walk with less severe breaks, so never rely on walking as a test of whether a bone has been fractured
-
Change in the appearance of the ankle – it will look different from the other ankle
-
Bone protruding through the skin—a sign of an emergency. Fractures that pierce the skin require immediate attention because they can lead to severe infection and prolonged recovery.
Diagnosis
Following an ankle injury it is important to have the ankle evaluated by a foot and ankle surgeon for proper diagnosis and treatment. If you are unable to do so right away, go to the emergency room and then follow up with a foot and ankle surgeon as soon as possible for a more thorough assessment.
The affected limb will be examined by the foot and ankle surgeon by touching specific areas to evaluate the injury. In addition, the surgeon may order x-rays and other imaging studies, as necessary.
Non-Surgical Treatment
Treatment of ankle fractures depends upon the type and severity of the injury. At first, the foot and ankle surgeon will want you to follow the R.I.C.E. protocol:
-
Rest: Stay off the injured ankle. Walking may cause further injury.
-
Ice: Apply an ice pack to the injured area, placing a thin towel between the ice and the skin. Use ice for 20 minutes and then wait at least 40 minutes before icing again.
-
Compression: An elastic wrap should be used to control swelling.
-
Elevation: The ankle should be raised slightly above the level of your heart to reduce swelling.
Additional treatment:
The treatment for a broken ankle usually involves a leg cast or brace if the fracture is stable. If the ligaments are also torn, or if the fracture created a loose fragment of bone that could irritate the joint, surgery may be required to secure the bones in place so they will heal properly or repair soft tissue injuries, if present. The foot and ankle surgeon will select the procedure that is appropriate for your injury.
Follow-up Care
It is important to follow your surgeon’s instructions after treatment. Failure to do so can lead to infection, deformity, arthritis, and chronic pain.
Foot Fracture: There are two types of foot fractures: stress fractures and general bone fractures. Stress fractures usually occur in the bones of the forefoot extending from the toes to the middle of the foot. Stress fractures are like tiny cracks in the bone surface. They can happen with sudden increases in exercise (such as running or walking for longer distances or times), improper training techniques, or a change in surfaces.
Stress Fractures: Incomplete cracks in bone caused by overuse. With complete rest, stress fractures in toes or any bones of the foot heal quickly. Extra padding in shoes can help prevent the condition. Left untreated, stress fractures may become complete bone fractures, which require casting and immobilization.
General Bone Fracture: Most other types of fractures extend through the bone, and are called bone fractures. They may be stable, in which there is no shift in bone alignment, or displaced, in which the bone ends no longer line up properly. Bone fractures usually result from trauma, such as dropping a heavy object on your foot, or from a twisting injury. If the fractured bone does not break through the skin, it is called a closed fracture. If the fracture does break through the skin, it is called an open fracture.
Foot Fracture: Nearly one-fourth of all the bones in your body are in your feet. A broken (fractured) bone in your forefoot or in one of your toes is often painful, but rarely disabling. Most of the time, these injuries heal without operative treatment.
Most other types of fractures extend through the bone, and are called bone fractures. They may be stable, in which there is no shift in bone alignment, or displaced, in which the bone ends no longer line up properly. Bone fractures usually result from trauma, such as dropping a heavy object on your foot, or from a twisting injury. If the fractured bone does not break through the skin, it is called a closed fracture. If the fracture does break through the skin, it is called an open fracture.
Because of the complex structures in the foot, there are some other, more specific types of fractures that can occur. For example, the fifth metatarsal, known as the little or pinky toe, is susceptible to a variety of different fractures. The relationship between the ankle and the foot can be compromised by an ankle-twisting injury, which may tear the tendon that attaches to this bone and pull a small piece of the bone away. A more serious injury in the same area is known as a Jones fracture, which occurs near the base of the bone and disrupts its blood supply. This injury may take longer to heal or require surgery.
Common symptoms for any type of foot fracture includes pain, swelling, and sometimes bruising. Be sure to seek medical attention for any suspected foot fracture.
Sports related Injuries:
Ankle Sprains, Achilles tendon disorders, heel pain, Morton’s Neuroma, Turf Toe, Stress fractures
From the repeated pounding that runners’ feet receive on paved surfaces to the side-to-side motion seen in court sports, there’s no question that athletes’ feet and ankles are prime candidates for injuries.
Ankle sprains – These are one of the most common sports injuries. Prompt evaluation and treatment by a foot and ankle surgeon is important… sometimes that “sprain” is actually an ankle fracture and treatment for these two conditions are very different. And don’t skimp on rehab! An ankle that has not been properly healed and strengthened is more likely to suffer repeated sprains, leading to chronic ankle instability.
Achilles tendon disorders – Athletes are at high risk for developing disorders of the Achilles tendon. Achilles tendonitis, an inflammation of the tendon that runs down the back of the lower leg, can progress into a degeneration of the tendon (Achillestendonosis). A sudden increase of a repetitive activity, leading to micro-injury of the tendon fibers, can cause these conditions.
Heel pain – This condition is most often caused by plantar fasciitis, although it may also be due to other causes including stress fractures. Although faulty foot structure is the most common cause of plantar fasciitis, it can also result from wearing shoes that are worn out or not designed for the sport in which you’re participating. Keeping the Achilles tendon stretched can help get rid of this pain, but continued pain should be checked out to rule out a fracture or other cause.
Morton’s neuroma – Also called “intermetatarsalneuroma,” this is a thickening of nerve tissue in the ball of the foot resulting from compression and irritation of the nerve. Causes include activities that involve repetitive irritation to the ball of the foot, such as running or court sports. Symptoms start gradually and may come and go when the nerve is irritated due to activity. But it’s important to have it treated early on before the damage becomes more severe.
Plantar Warts:
Most foot warts are harmless, even though they may be painful. They are often mistaken for corns or calluses, which are layers of dead skin that build up to protect an area which is being continuously irritated. A wart, however, is caused by a viral infection which invades the skin through small or invisible cuts and abrasions. Foot warts are generally raised and fleshy and can appear anywhere on the foot or toes. Occasionally, warts can spontaneously disappear after a short time, and then, just as frequently, they recur in the same location. If left untreated, warts can grow to an inch or more in circumference and can spread into clusters of warts. Children, especially teenagers, tend to be more susceptible to warts than adults.
Plantar warts, also known asverrucas, appear on the soles of the feet and are
one of several soft tissue conditions that can be quite painful. Unlike other foot
warts, plantar warts tend to be hard and flat, with a rough surface and well-
defined boundaries. They are often gray or brown (but the color may vary),
with a center that appears as one or more pinpoints of black. Plantar warts
are often contracted by walking barefoot on dirty surfaces or littered ground.
The virus that causes plantar warts thrives in warm, moist environments, making
infection a common occurrence in public pools and locker rooms.
Like any other infectious lesion, plantar warts are spread by touching, scratching,
or even by contact with skin shed from another wart. The wart may also bleed,
another route for spreading. Plantar warts that develop on the weight-bearing
areas of the foot (the ball or heel of the foot) can cause a sharp, burning pain.
Pain occurs when weight is brought to bear directly on the wart, although pressure
on the side of a wart can create equally intense pain.
To prevent the spread of warts, follow these tips:
-
Avoid direct contact with warts, both from other persons or from other parts of the body.
-
Avoid walking barefoot, except on sandy beaches.
-
Change your shoes and socks daily.
-
Check your children's feet periodically.
-
Keep your feet clean and dry.
It is important to note that warts can be very resistant to treatment and have a tendency to recur. Over-the-counter foot wart treatments are usually ineffective because their use can inadvertently destroy surrounding healthy tissue. Please contact our office for help in effectively treating warts. Our practice is expert in recommending the best treatment for each patient, ranging from prescription ointments or medications to, in the most severe cases, laser cautery.
What is a Plantar Wart?
A wart is a small growth on the skin that develops when the skin is infected by a virus. Warts can develop anywhere on the foot, but typically they appear on the bottom (plantar side) of the foot. Plantar warts most commonly occur in children, adolescents, and the elderly.
There are two types of plantar warts:
-
A solitary wart is a single wart. It often increases in size and may eventually multiply, forming additional “satellite” warts.
-
Mosaic warts are a cluster of several small warts growing closely together in one area. Mosaic warts are more difficult to treat than solitary warts.
Causes
Plantar warts are caused by direct contact with the human papilloma virus (HPV). This is the same virus that causes warts on other areas of the body.
Symptoms
The symptoms of a plantar wart may include:
-
Thickened skin. Often a plantar wart resembles a callus because of its tough, thick tissue.
-
Pain. Walking and standing may be painful. Squeezing the sides of the wart may also cause pain.
-
Tiny black dots. These often appear on the surface of the wart. The dots are actually dried blood contained in the capillaries (tiny blood vessels).
Plantar warts grow deep into the skin. Usually this growth occurs slowly, with the wart starting small and becoming larger over time.
Diagnosis and Treatment
To diagnose a plantar wart, the foot and ankle surgeon will examine the patient’s foot and look for signs and symptoms of a wart.
Although plantar warts may eventually clear up on their own, most patients desire faster relief. The goal of treatment is to completely remove the wart.
The foot and ankle surgeon may use topical or oral treatments, laser therapy, cryotherapy (freezing), acid treatments, or surgery to remove the wart.
Regardless of the treatment approaches undertaken, it is important that the patient follow the surgeon’s instructions, including all home care and medication that has been prescribed, as well as follow-up visits with the surgeon. Warts may return, requiring further treatment.
If there is no response to treatment, further diagnostic evaluation may be necessary. In such cases, the surgeon can perform a biopsy to rule out other potential causes for the growth.
Although there are many folk remedies for warts, patients should be aware that these remain unproven and may be dangerous. Patients should never try to remove warts themselves. This can do more harm than good.
Osteoarthritis of the Foot and Ankle
What Is Osteoarthritis?
Osteoarthritis is a condition characterized by the breakdown and eventual loss of cartilage in one or more joints. Cartilage (the connective tissue found at the end of the bones in the joints) protects and cushions the bones during movement. When cartilage deteriorates or is lost, symptoms develop that can restrict one’s ability to easily perform daily activities.
-
Osteoarthritis is also known as degenerative arthritis, which may develop as part of the aging process..
-
Osteoarthritis appears in the foot, most frequently, in the big toe, although it is also often found in themidfootand ankle.
Causes
-
Repeated stress and use of the affected joint over time. As the cartilage deteriorates and gets thinner, the bones lose their protective covering and eventually may rub together, causing pain and inflammation of the joint.
-
A previous fracture or soft tissue injury around the joint
-
Abnormal foot mechanics such as flat feet or high arches.
Osteoarthritis in the big toe is often caused by kicking or jamming the toe, or by dropping something on the toe. Osteoarthritis in themidfootis often caused by dropping something on it, or by a sprain or fracture. In the ankle, osteoarthritis is usually caused by a fracture and occasionally by a severe sprain.
Symptoms
People with osteoarthritis in the foot or ankle experience, in varying degrees,
one or more of the following:
-
Pain and stiffness in the joint
-
Swelling in or near the joint
-
Difficulty walking or bending the joint
-
New unwanted bone growth from shoe pressure. Can result in calluses,
corns or blisters. Bone spurs can also limit the movement of the joint.
Diagnosis
In diagnosing osteoarthritis, the foot and ankle surgeon will examine the foot thoroughly, looking for swelling in the joint, limited mobility, and pain with movement. In some cases, deformity and/or enlargement (spur) of the joint may be noted. X-rays may be ordered to evaluate the extent of the disease.
Non-surgical Treatment
-
To help relieve symptoms, the surgeon may begin treating osteoarthritis with one or more of the following non-surgical approaches:
-
Oral medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, are often helpful in reducing the inflammation and pain. Occasionally a prescription for a steroid medication is needed to adequately reduce symptoms.
-
Orthotic devices. Custom orthotic devices (shoe inserts) are often prescribed to provide support to improve the foot’s mechanics or cushioning to help minimize pain.
-
Bracing. Bracing, which restricts motion and supports the joint, can reduce pain during walking and help prevent further deformity.
-
Immobilization. Protecting the foot from movement by wearing a cast or removable cast-boot may be necessary to allow the inflammation to resolve.
-
Steroid injections. In some cases, steroid injections are applied to the affected joint to deliver anti-inflammatory medication.
-
Physical therapy. Exercises to strengthen the muscles, especially when the osteoarthritis occurs in the ankle, may give the patient greater stability and help avoid injury that might worsen the condition.
Surgical Treatment:
When osteoarthritis has progressed substantially or failed to improve with non-surgical treatment, surgery may be recommended. In advanced cases, surgery may be the only option. The goal of surgery is to decrease pain and improve function. The foot and ankle surgeon will consider a number of factors when selecting the procedure best suited to the patient’s condition and lifestyle.
Gout:
What Is Gout?
Gout is a disorder that results from the build-up of uric acid in the tissues or a joint.
It most often affects the joint of the big toe.
Causes
Gout attacks are caused by deposits of crystallized uric acid in the joint. Uric acid is
present in the blood and eliminated in the urine, but in people who have gout, uric
acid accumulates and crystallizes in the joints. Uric acid is the result of the break-
down of purines, chemicals that are found naturally in our bodies and in food. Some
people develop gout because their kidneys have difficulty eliminating normal amounts of uric acid, while others produce too much uric acid.
Gout occurs most commonly in the big toe because uric acid is sensitive to temperature changes. At cooler temperatures, uric acid turns into crystals. Since the toe is the part of the body that is farthest from the heart, it’s also the coolest part of the body – and, thus, the most likely target of gout. However, gout can affect any joint in the body.
The tendency to accumulate uric acid is often inherited. Other factors that put a person at risk for developing gout include: high blood pressure, diabetes, obesity, surgery, chemotherapy, stress, and certain medications and vitamins. For example, the body’s ability to remove uric acid can be negatively affected by taking aspirin, some diuretic medications (“water pills”), and the vitamin niacin (also called nicotinic acid). While gout is more common in men aged 40 to 60 years, it can occur in younger men as well as in women.
Consuming foods and beverages that contain high levels of purines can trigger an attack of gout. Some foods contain more purines than others and have been associated with an increase of uric acid, which leads to gout. You may be able to reduce your chances of getting a gout attack by limiting or avoiding shellfish, organ meats (kidney, liver, etc.), red wine, beer, and red meat.
Symptoms
An attack of gout can be miserable, marked by the following symptoms:
-
Intense pain that comes on suddenly – often in the middle of the night or upon
arising
-
Signs of inflammation such as redness, swelling, and warmth over the joint.


Gout
Neuroma:
Neuroma – This condition is caused by a thickening of the nerve that runs between any two toes either by trauma or as a result of an abnormality of the foot. Neuromas most often in the ball of the foot, causing a pinched and inflamed nerve.
What is a neuroma?
-
Neuromas—enlarged benign growths of nerves, most commonly between the third and fourth toes. Neuromas are caused by tissue rubbing against and irritating the nerves. Pressure from ill-fitting shoes or abnormal bone structure can also lead to this condition.
-
Treatment: Depending on the severity, treatments may include orthotics (shoe inserts), cortisone injections, and, in extreme cases, surgical removal of the growth.
-
During neuroma procedures, an incision is made on the top of the foot in the location of the neuroma, usually between the second and third toes or between the third and fourth toes. After the nerve is located, the surgeon cuts and removes it.

